.tmb-768v.png?Culture=en&sfvrsn=54737d84_1)
Virtual primary care use during the COVID-19 pandemic: lessons for a post-pandemic world
Key learning themes
The initial phase of the COVID-19 pandemic demonstrated the value of virtual health care as a key service delivery model in the context of the primary care setting.
• For patients, virtual health care allowed for continued access to essential primary care services, alleviated isolation for some vulnerable patient groups and empowered others towards achieving greater self-care, all the while ensuring physical distancing to limit COVID-19 transmission. However, health inequities, digital exclusion, communication difficulties, and patient preferences and experiences, are all challenges which need to be addressed.
• For health care providers, virtual care tools were a convenient way of enabling primary care delivery and triage, enhance communication with other health care workers, and provide greater work flexibility. Simultaneously, clinical uncertainty, due to the inability to examine patients in person, the lack of sufficient guidance and support, higher workloads, issues with remuneration and the unsuitability of this modality of consultation for certain clinical presentations, are all problems which need to be considered when implementing virtual primary care tools in the future.
• For health care administrators and policy makers, establishing longterm, sustainable funding schemes, mandating data interoperability in future systems and enacting more robust supporting regulatory legislation surrounding patient data protection, are all necessary steps for ensuring that virtual primary care is and remains a safe way of delivering care.
• Based on these findings, a framework for the implementation of virtual primary care has been developed, considering five key domains: contextual considerations; technology infrastructure; awareness and experience; safety and risk management; strategic planning; and supporting policies. Quality standards across these domains should be longitudinally monitored using mixed methods, both capturing qualitative perceptions from users, and realworld key performance metrics.
Context
This learning brief draws on findings derived from several publicly available peerreviewed articles. For further details, please refer to the end of the brief.
Prior to the onset of COVID-19, virtual primary care – a broad term describing the use of phone or digital technologies to enable primary care activities – was largely a nascent technology. While slowly increasing in availability over the years, virtual primary care had remained a complementary or alternative means to face-to-face consultations.
The COVID-19 pandemic changed all that as it presented health systems worldwide with a set of unprecedented challenges. Virtual approaches rapidly became the mainstay modality for health care delivery during the early phases of the pandemic, supporting continuity of care, facilitating public health interventions and disease surveillance, and curbing disease transmission in the community.
This abrupt and rapid adoption of virtual primary care has had significant implications on the care received by patients, the health provider’s routine clinical practice, and has pushed health systems towards greater incorporation of virtual primary care as an important means of care delivery, moving on from the pandemic.
This briefing aims to summarize the key findings from the experiences of primary care physicians using virtual care tools. Using an online survey, we explored the perspectives of general practitioners working during the COVID-19 pandemic (June-September 2020) across 20 countries, and invited them to share their views on the main barriers and challenges of using virtual care.
Benefits of virtual primary care
Throughout the pandemic, virtual care tools helped resolve the tension between the need to ensure access to care, while complying with physical distancing restrictions to limit the transmission of COVID-19, thus playing a key role in guaranteeing continuity of primary care delivery. This benefit was noted as particularly relevant to some specific vulnerable patient groups, such as the elderly, and those with mobility issues.
Remote triage allowed for a reduction of unnecessary in-person doctor visits and the prioritization of those who needed face-to-face care. This positively contributed to both improving timeliness and efficiency of care.
Technology also enhanced communication between health care providers and contributed positively to patients’ care experience by increasing convenience, self-care awareness for minor illnesses, and instilling a greater sense of patient empowerment. Concerning benefits, it is also important to note the transforming impact that virtual care tools have had in hastening the digital transformation of primary care and their associated legal and regulatory frameworks.
However, the increased level of access must also be balanced with health care provider workloads. Physician experiences during the pandemic have highlighted the frequency and ease with which patients could contact their primary care physician, often blurring the boundaries between their work and personal lives. This often resulted in less engaged interactions during consultations, impairing the physician-patient relationship, decreased work satisfaction, and contributed to physician burnout.
Challenges of virtual primary care
While virtual primary care provided an additional means to accessing care, during the pandemic, for many patients, it became the sole means of doing so. Vulnerable patients, particularly those with lower digital literacy, or those without access to reliable equipment, risked digital exclusion. Those who preferred face-to-face consultations were often not offered alternatives to virtual care.
Primary care physicians also noted the potential negative impact of providing care in the absence of a physical examination, including concerns about increased clinical uncertainty, risk of misdiagnosis and delays in diagnosis and treatment. Other challenges identified include a lack of formal guidance, remuneration issues, resistance to organizational change, technical difficulties, implementation and financial issues, and regulatory weaknesses. Finally, it was highlighted that remote care is simply unsuitable for certain types of consultations and patients.
As virtual primary care increases in prevalence in the post-pandemic world, considerable efforts must be made to ensure that it does not result in an inadvertent entrenching and exacerbation of existing health inequities.
Based on the benefits and challenges identified, we propose a framework of recommendations for the implementation of safe, high-quality primary care across five main domains: technology infrastructure, awareness and experience, safety and risk management, strategic planning and supporting policies (Figure 1). The factors identified stress the importance of accounting for context in which virtual care tools are to be deployed, and underscore the need to incrementally develop, implement and evaluate tailored strategies to address the challenges identified at the local level.
The need for continuous, responsive and adaptative monitoring of metrics across these five areas is a cross-dimensional imperative. We recommend that monitoring be performed through data collection from a variety of sources, including both patient and provider feedback, and real-word data from routinely collected health data.
Virtual primary care is now faced with the challenge of needing to evolve into its best version, in a continuously changing landscape. Looking ahead, platforms will need to be more accessible, secure and reliable – yet flexible enough to rapidly adapt to patients’ and providers’ dynamic preferences, organizational requirements and processes, and account for a myriad of technological and regulatory considerations. Ultimately, virtual primary care must be aligned with the greater primary care values and be delivered in a way that is sustainable, respects user preferences, while remaining centred on patient’s evolving needs throughout their lives.
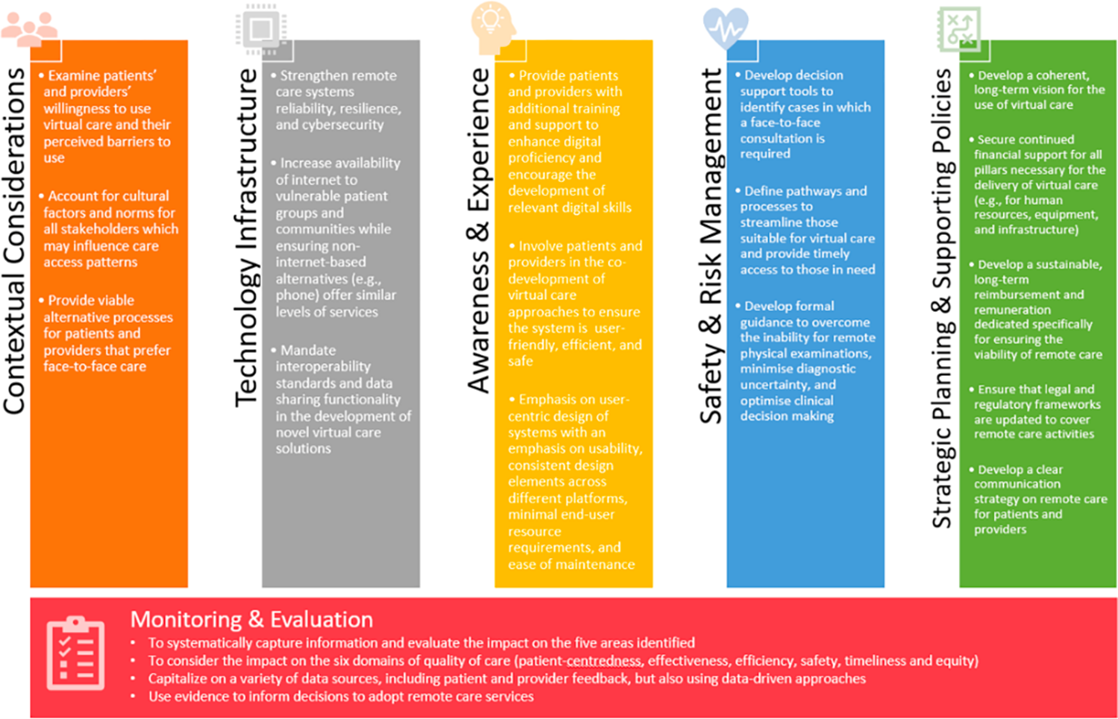
Figure 1: A framework of recommendation for implementation of safe, effective virtual primary care
Further reading
Disclaimer


